Blog
Autoimmune Conditions and Peptide Therapy: Hope or Hype?

Autoimmune disorders affect millions and can strike any organ. When the immune system attacks the body, it creates a chronic illness.
Patients search for relief beyond conventional drugs that often bring side effects. Peptide therapy has emerged as a promising frontier for people tired of medications that only manage symptoms.
In this post, we explore the science, benefits, and uncertainties of peptide therapy for autoimmune disease.
We examine key peptides, current evidence, and what you should consider before starting any regimen.
Our goal is to answer your burning questions and provide a balanced view so you can make informed decisions.
In This Article
- Understanding Autoimmune Conditions
- Limitations of Current Treatments
- How Does Peptide Therapy Work?
- Spotlight on Key Peptides
- The Gut‑Immune Connection
- Safety, Legality, and Ethical Considerations
- Integrative Approach: Lifestyle and Other Therapies
- Hope or Hype? Evaluating the Evidence
- Conclusion
Understanding Autoimmune Conditions
Autoimmune diseases arise when the immune system mistakenly attacks healthy cells instead of invaders.
This misfire causes chronic inflammation and tissue damage. More than eighty types of autoimmune disorders exist, such as rheumatoid arthritis, lupus, multiple sclerosis, and type 1 diabetes.
Each disease has different symptoms, yet all share an overactive immune response. Genetics, environmental triggers, and infections contribute to this misdirected immunity.
With modern lifestyles changing rapidly, our immune systems may be confused by processed foods, pollutants, and stress.
What causes autoimmune disorders?
Scientists are still unraveling why the immune system turns against the body. Common hypotheses point to genetic predisposition plus environmental triggers.
Viral or bacterial infections can prime the immune system to recognize the self as foreign. Exposure to toxins, chemicals, or heavy metals may also disrupt immune tolerance.
Diet and gut health play a huge role: an imbalanced microbiome can trigger inflammation that spills into systemic disease.
Hormonal changes during puberty, pregnancy, or menopause can modulate immune function and spark disease onset.
Stress is another known trigger that may push susceptible individuals into an autoimmune state.
Common symptoms and diseases
Because the immune system can attack any organ, the symptoms of autoimmune disease vary widely.
Common signs include fatigue, muscle or joint pain, skin rashes, and digestive issues. Some people experience recurrent fevers, brain fog, or nerve pain.
Specific diseases attack particular organs: multiple sclerosis targets nerves, lupus affects connective tissue, and inflammatory bowel diseases harm the gut.
Many patients cycle through years of vague complaints before receiving a diagnosis. The broad range of symptoms makes autoimmune conditions hard to detect early.
Raising awareness and recognizing patterns can help people seek help sooner.
Limitations of Current Treatments
Doctors rely on immunosuppressive drugs, corticosteroids, and biologic therapies to manage autoimmune disease.
These treatments aim to reduce inflammation and relieve symptoms. Common medications include corticosteroids, methotrexate, anti‑TNF antibodies, and intravenous immunoglobulin.
They can provide relief but often come with serious side effects like infections, weight gain, mood swings, and bone loss.
Biologic drugs target specific immune pathways, but patients may still suffer opportunistic infections and long‑term risks like cancer.
Many drugs require continuous use and lose effectiveness over time. Because there is no cure, patients must balance symptom control against the burden of side effects.
This reality drives interest in alternative therapies.
How Does Peptide Therapy Work?
Peptides are short chains of amino acids that act as signaling molecules in the body. They regulate hormones, immune responses, and tissue repair.
Peptide therapy involves administering specific sequences to modulate biological functions. Advocates believe peptides can fine‑tune immunity without broadly suppressing it.
For autoimmune conditions, the goal is to calm hyperactive immune responses while promoting healing. Certain peptides may stimulate regulatory T cells, reduce inflammatory cytokines, or support tissue regeneration.
Because peptides mimic natural signals, they are thought to have fewer side effects than drugs. However, most therapeutic peptides are considered experimental and are not approved by the U.S. Food and Drug Administration for treating autoimmune disease.
Peptides can be delivered via injection, nasal spray, or oral lozenges. They are typically taken in cycles under medical supervision.
The mechanism depends on the specific peptide: some enhance immune surveillance; others promote blood vessel growth or collagen synthesis.
For example, Thymosin Alpha‑1 boosts T cell function and has been studied for sepsis and viral infections.
BPC‑157 appears to support the gut lining and reduce inflammation in animal models. KPV reduces inflammatory signaling in intestinal cells
Understanding each peptide’s action helps guide appropriate use. Consultation with a qualified healthcare provider is essential.
Spotlight on Key Peptides
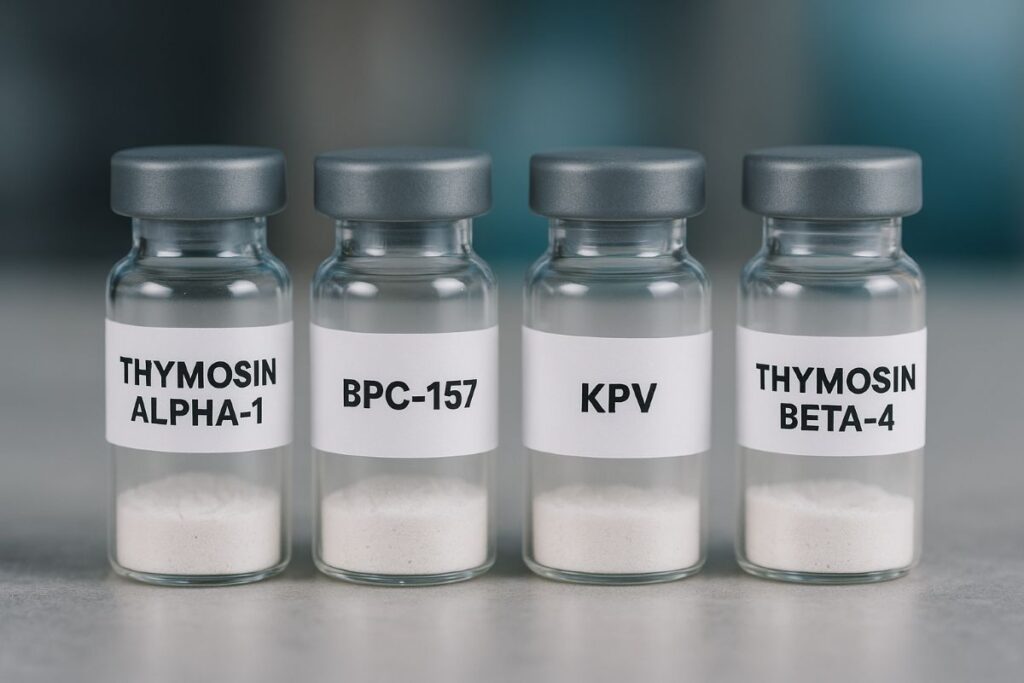
The world of peptides is vast, but a few candidates are making headlines for autoimmune conditions.
We explore four peptides that have attracted attention: Thymosin Alpha‑1, BPC‑157, KPV, and Thymosin Beta 4. Each has unique properties, potential benefits, and caveats.
Keep in mind that evidence is preliminary and largely based on animal studies or small human trials. It is vital to use these peptides under professional guidance and in combination with other supportive therapies.
Thymosin Alpha‑1: modulating immunity
Thymosin Alpha‑1 (TA‑1) is a 28‑amino‑acid peptide derived from prothymosin alpha. It plays a key role in the maturation of T cells and cell‑mediated immunity.
TA‑1 is approved in several countries for treating viral infections and has been used as an adjunct therapy in cancer and chronic hepatitis.
Research shows that TA‑1 enhances the expression of IL‑2 receptors and supports the proliferation of helper T cells.
In sepsis models, it reduces mortality and improves immune responsiveness. Some clinicians use TA‑1 off‑label to support patients with autoimmune disease, citing its ability to modulate the immune system without broad suppression.
Despite promising data, TA‑1 remains experimental for autoimmune conditions. Most studies involve small sample sizes or focus on infections rather than autoimmunity.
TA‑1 is generally well tolerated. Common side effects are mild injection‑site reactions. Serious adverse events occur mainly when it is combined with interferon therapy.
Importantly, TA‑1 is not approved by the FDA for autoimmune treatment, so patients should seek medical supervision and consider legal implications.
Some clinics offer TA‑1 as part of a wellness program. When exploring TA‑1, ask about dosing, expected outcomes, and how it fits within your overall care plan.
BPC‑157: healing and anti‑inflammatory properties
BPC‑157 is a 15‑amino‑acid fragment derived from a gastric protein. It has gained popularity for promoting tissue repair and reducing inflammation.
Animal studies show that BPC‑157 accelerates the healing of tendons, ligaments, and the gut lining. It enhances angiogenesis and upregulates vascular endothelial growth factor (VEGF), which increases blood supply to injured tissues.
In rat models of polyarthritis, BPC‑157 reduced paw swelling, inflammation, and stiffness. These properties suggest potential benefits for autoimmune diseases that damage joints or gut mucosa.
Although BPC‑157 shows promise in animals, human data are scarce. A systematic review found no acute toxicity in animals and no adverse events across various doses.
However, there are no large clinical trials examining its safety or efficacy in autoimmune patients. The peptide is not FDA‑approved, and quality control varies among compounding pharmacies.
People interested in BPC‑157 should consult qualified practitioners and monitor for any adverse reactions.
Our own discussion of BPC‑157’s mechanism can be found in an in‑depth article on the healing peptide mechanism.
KPV peptide: targeting gut inflammation
KPV is a tripeptide composed of lysine, proline, and valine. It is a segment of the hormone alpha‑melanocyte‑stimulating hormone and exhibits potent anti‑inflammatory effects. In laboratory studies, KPV reduces activation of NF‑κB and MAPK pathways, which are central to inflammatory responses.
When administered orally in mouse models of colitis, KPV significantly decreased colon inflammation and improved disease severity.
These findings indicate KPV may protect the gut lining and modulate immune signaling.
KPV appears to exert its effects via the peptide transporter PepT1 rather than classical melanocortin receptors.
By entering cells through PepT1, KPV reduces pro‑inflammatory cytokine secretion and oxidative stress. Early clinical use suggests minimal side effects, though injection‑site irritation or mild gastrointestinal upset can occur.
People with inflammatory bowel disease or systemic inflammation may find KPV appealing. To learn more about this anti‑inflammatory peptide, check out our product page on gut support peptide.
Thymosin Beta 4: potential role in rheumatoid arthritis
Thymosin Beta 4 (Tβ4) is a ubiquitous peptide involved in cell migration, angiogenesis, and wound repair. Researchers noticed elevated levels of Tβ4 in the serum and synovial fluid of patients with rheumatoid arthritis.
This suggests Tβ4 might play a role in disease pathogenesis or tissue repair. In animal models, Tβ4 promotes regeneration of injured tissues and may protect against fibrosis. Some theorize that supplementing Tβ4 could support joint healing and reduce inflammation.
Despite its intriguing properties, the role of Tβ4 in autoimmune disease remains unclear. Elevated levels could reflect a protective response to injury rather than a causal factor.
Currently, there is limited research on exogenous Tβ4 administration in humans with autoimmune disease.
More studies are needed to understand its safety, optimal dosing, and therapeutic potential. If you’re curious about the synergy between BPC‑157 and Tβ4, explore our article on the wolverine stack.
The Gut‑Immune Connection
The gut houses trillions of microbes that educate the immune system. This microbiota helps distinguish friend from foe and maintains immune tolerance.
Dysbiosis, or imbalance of gut flora, is linked to autoimmune disease development. Diet, antibiotic use, stress, and infections can disrupt the microbial ecosystem.
When harmful bacteria dominate, the intestinal barrier becomes leaky. Undigested food particles and toxins may escape into the bloodstream, triggering inflammation throughout the body.
Peptides may influence the gut‑immune axis. BPC‑157 helps repair the intestinal lining and supports healthy gut flora.
KPV directly reduces inflammatory signaling in intestinal cells. By supporting barrier integrity and reducing inflammation, these peptides may decrease autoimmune triggers originating in the gut.
Improving diet, increasing fiber and fermented foods, and avoiding processed ingredients are also critical.
Combining gut‑focused peptides with lifestyle changes and probiotics can create a holistic approach to restoring immune balance.
Safety, Legality, and Ethical Considerations
Peptide therapy for autoimmune disease remains largely experimental. Most peptides described here are not approved by the FDA for treating autoimmune conditions.
They are often compounded by pharmacies under the guidance of healthcare providers. Because of lax regulation, purity and dosing can vary widely.
Patients should only source peptides from reputable clinics and consult licensed practitioners.
Research shows peptides like Thymosin Alpha‑1 are generally well-tolerated with minor side effects. BPC‑157 has shown no toxicity in animal studies, but human safety is uncertain.
KPV appears safe but may cause mild injection‑site irritation or gastrointestinal upset. Thymosin Beta 4’s effects are not fully understood.
Pregnant or nursing women and individuals with severe immune suppression should avoid experimental peptides.
Ethical issues arise when products are marketed as cures without sufficient evidence. Always discuss therapies with your doctor and avoid unsupervised self‑administration.
Integrative Approach: Lifestyle and Other Therapies
Peptides may offer hope, but they should complement—not replace—conventional treatments and healthy habits.
Lifestyle modifications are fundamental in managing autoimmune disease. Regular exercise improves joint flexibility and mood, while stress reduction practices like meditation can calm the immune system.
A nutrient‑dense diet rich in fruits, vegetables, and omega‑3 fats supports gut health and reduces inflammation.
Eliminating triggers like gluten, dairy, or processed sugars may benefit some individuals. Adequate sleep, sunlight, and hydration also play key roles.
Conventional therapies like physical therapy, occupational therapy, and intravenous immunoglobulin remain important.
Integrative practitioners may recommend antioxidant IV drips, ozone therapy, or personalized supplement regimens.
Our clinic offers a range of services, from vitamin shots to immune support drips that can be tailored to your needs.
Combining evidence‑based medicine with supportive therapies and mindful lifestyle choices offers the best chance at long‑term wellness.
Always consult your healthcare team before integrating new therapies.
Hope or Hype? Evaluating the Evidence
The excitement around peptide therapy reflects a desire for safer, more targeted treatments. Early studies suggest peptides can modulate immune responses, promote tissue repair, and improve gut integrity.
However, most evidence comes from animal models or small human trials. There is a lack of large randomized clinical studies evaluating the effectiveness in autoimmune diseases.
Without robust data, it is hard to distinguish hope from hype. Peptides are not magic bullets. They may provide incremental benefits when used appropriately and under supervision.
Overblown claims and self‑administration can lead to disappointment or harm. When evaluating peptides, consider the quality of evidence, personal health history, and your healthcare provider’s guidance.
Ask whether there are published studies, what outcomes were measured, and whether results apply to your condition.
Remain cautious of marketing that promises cures or uses pseudoscience. Balanced optimism will help you navigate the emerging field of peptide therapy.
Conclusion
Autoimmune conditions are complex and demand a multifaceted approach. Peptide therapy offers intriguing possibilities but remains in the early stages of research.
Evidence suggests that peptides like Thymosin Alpha‑1, BPC‑157, KPV, and Thymosin Beta 4 can modulate immune responses, promote healing, and support gut health.
Yet these therapies should be viewed as adjuncts, not replacements for established treatments. As you explore options, maintain realistic expectations and seek professional guidance.
Prioritize lifestyle habits that reduce inflammation and support overall wellness. Recognize that managing autoimmune disease is a journey requiring patience, experimentation, and collaboration with healthcare providers.
With informed choices and integrative care, you can harness the potential of peptide therapy while staying grounded in science.