Blog
Hormone Imbalance Symptoms and Testing: How to Know When It’s Time to Check Your Levels

That constant fatigue you’ve been blaming on work. The stubborn weight that won’t budge despite eating well. The mood swings seem to come from nowhere. The nights you can’t sleep, even though you’re exhausted. These aren’t just signs of getting older—they may be hormone imbalance symptoms telling you something needs attention.
Hormones control nearly every system in your body. When they fall out of balance, the effects ripple through your energy, mood, metabolism, sleep, and sex drive. The tricky part? These symptoms often appear gradually, making it easy to dismiss them as stress, aging, or just “how things are now.”
This guide walks through the most common hormone imbalance symptoms in both men and women, when hormone testing makes sense, and how LIVV Natural helps patients move from confusion to clarity—and from testing to treatment that actually works.
Common Signs of Hormone Imbalance You Shouldn’t Ignore
Hormonal shifts affect people differently depending on age, sex, and which hormones are involved. Some symptoms overlap between men and women; others are more specific. Here’s what to watch for:
Persistent Fatigue That Sleep Doesn’t Fix
Everyone gets tired. But if you wake up exhausted after eight hours of sleep, feel drained by mid-afternoon despite caffeine, or lack the energy to do activities you used to enjoy—that’s different.
Low thyroid hormone, declining testosterone, elevated cortisol, or disrupted adrenal function can all cause this pattern. The TRAVERSE clinical trial found that men with confirmed low testosterone who received hormone therapy experienced measurable improvements in energy levels and hypogonadal symptoms over two years.
Fatigue that doesn’t respond to rest, better sleep habits, or lifestyle changes warrants hormone testing.
Unexplained Weight Changes
Gaining weight despite sticking to your usual diet and exercise routine—or losing weight without trying—suggests your metabolism isn’t functioning normally.
Thyroid hormones regulate metabolic rate. Low thyroid (hypothyroidism) slows everything down, making weight loss difficult and weight gain likely. High thyroid (hyperthyroidism) speeds things up, sometimes causing weight loss alongside anxiety and rapid heartbeat.
Cortisol, the stress hormone, promotes fat storage—especially around the midsection—when chronically elevated. Insulin resistance, often tied to hormonal dysfunction, makes the body store rather than burn calories.
If your scale keeps moving despite consistent habits, your hormones may be the hidden variable.
Mood Swings, Anxiety, and Low Mood
Hormones directly influence brain chemistry. Estrogen, progesterone, testosterone, and thyroid hormones all affect neurotransmitters like serotonin and dopamine that regulate mood.
Women often notice mood changes around their menstrual cycle, during perimenopause, or after menopause. Fluctuating estrogen and progesterone levels create emotional instability, irritability, or feelings of depression.
Men with declining testosterone frequently report low mood, irritability, and reduced motivation. Research on androgen deficiency has documented that partial testosterone deficiency in aging men correlates with depressive symptoms, anxiety, and decreased psychological vitality.
When mood changes persist without a clear cause—and don’t respond to typical interventions—hormone testing can reveal whether biochemistry is the driver.
Reduced Libido and Sexual Dysfunction
Sex drive depends heavily on hormones. Testosterone drives desire in both men and women. Estrogen supports vaginal health and arousal in women. Thyroid hormones affect energy and overall function.
Men experiencing low testosterone often notice decreased interest in sex, difficulty achieving or maintaining erections, and reduced satisfaction. The TRAVERSE study showed that testosterone therapy significantly improved sexual activity scores and desire in men with hypogonadism.
Women with hormonal changes—particularly during perimenopause and menopause—may experience vaginal dryness, painful intercourse, and reduced desire. Low testosterone in women (yes, women need it too) contributes to decreased libido and arousal difficulty.
If your sex life has changed noticeably without relationship or stress factors explaining it, hormones deserve investigation.
Sleep Disturbances
Hormones regulate your sleep-wake cycle. Cortisol should peak in the morning to wake you up and drop at night to let you sleep. Melatonin rises in the evening. When these patterns break down, so does your sleep.
High cortisol at night keeps you wired when you should be winding down. Low progesterone can cause restless sleep in women. Thyroid dysfunction disrupts sleep quality. Hot flashes and night sweats—classic signs of declining estrogen—interrupt sleep multiple times per night.
Chronic poor sleep then worsens other hormone imbalance symptoms by increasing cortisol and inflammation while decreasing testosterone and growth hormone production. It becomes a self-reinforcing cycle.
Physical Changes: Hair, Skin, and Body Composition
Hormones influence what you see in the mirror. Men with low testosterone may notice loss of muscle mass, increased body fat, and reduced body hair. Women with hormonal shifts often experience hair thinning, dry skin, or adult acne.
Thyroid dysfunction commonly causes hair loss, dry skin, and brittle nails. Women may notice heavier or irregular periods, while men might see changes in beard growth or chest hair.
These visible changes often accompany the internal symptoms, providing additional clues that hormone levels need evaluation.
When to Consider Testing Your Hormone Levels
Not every bout of fatigue or bad mood means your hormones are off. But certain patterns warrant testing.
Multiple Symptoms Occurring Together
One symptom could have many explanations. Three or four symptoms—fatigue plus weight gain plus low mood plus poor sleep—pointing in the same direction suggest a systemic issue like hormone imbalance.
If you checked several items on the symptom list above, a comprehensive blood panel covering thyroid function, sex hormones, and stress markers makes sense.
Symptoms Persisting Despite Lifestyle Changes
You’ve improved your sleep. You’re exercising. You’re eating better. You’ve reduced stress where possible. And nothing changes.
When symptoms persist despite doing the right things, the answer often lies in biochemistry rather than behavior. Hormone testing can identify what lifestyle alone can’t fix.
Men in Their 30s and Beyond With Low T Symptoms
Testosterone naturally declines with age—about 1-2% per year after age 30. By 40 or 50, some men experience levels low enough to cause symptoms.
Signs suggesting low testosterone include reduced libido, erectile difficulties, fatigue, loss of muscle mass, increased body fat, and decreased motivation. Men’s hormone optimization starts with accurate testing to confirm whether testosterone is actually low and to identify contributing factors.
A morning blood test measuring total and free testosterone, along with SHBG, estradiol, and LH/FSH, provides a complete picture.
Women With Perimenopause or Menopause Symptoms
Women in their late 30s through 50s may experience hormonal shifts even before their periods stop completely. Perimenopause can last years, with irregular cycles, hot flashes, mood changes, and sleep disruption.
Testing estrogen, progesterone, FSH, and thyroid hormones helps distinguish perimenopause from other conditions and guides treatment decisions. Women’s hormone therapy options range from bioidentical hormone replacement to natural support depending on symptoms and lab findings.
Thyroid or Adrenal Symptoms
Cold sensitivity, constipation, dry skin, and sluggish metabolism suggest thyroid involvement. Ongoing fatigue paired with high stress, poor stress recovery, and sleep-wake cycle disruption points toward cortisol and adrenal issues.
Targeted testing—thyroid panel (TSH, Free T3, Free T4, antibodies) or cortisol evaluation (blood or saliva at multiple time points)—can confirm or rule out these causes.
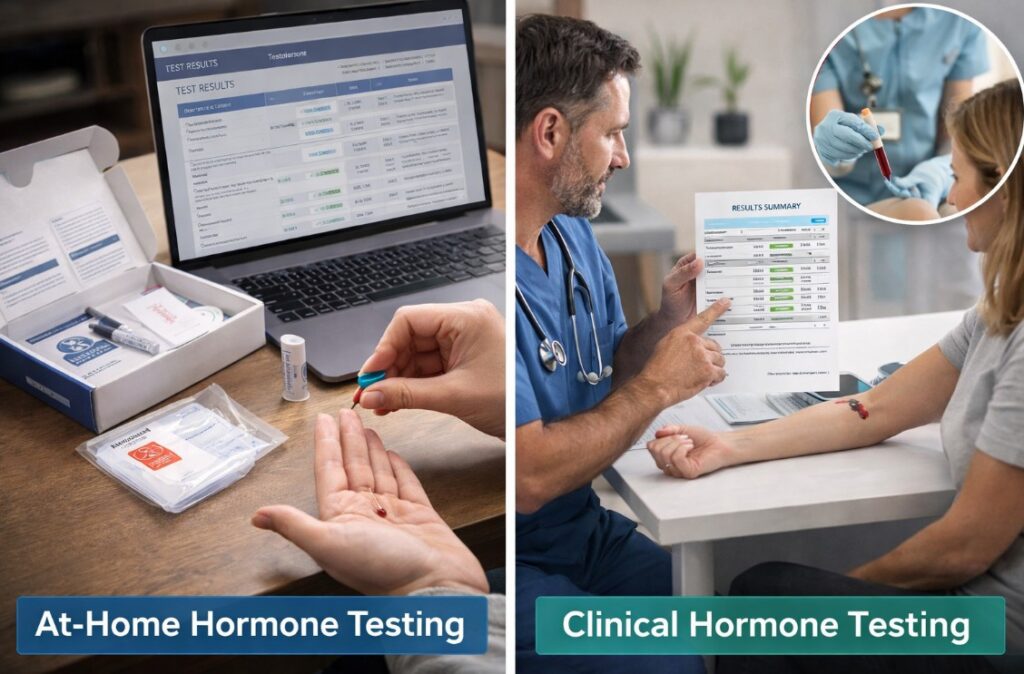
At-Home vs Clinical Hormone Testing
At-home hormone test kits have become widely available, offering convenience and privacy. But they come with limitations worth understanding.
At-Home Testing: Convenience With Caveats
Mail-in hormone kits let you collect samples—usually finger-prick blood or saliva—at home and send them to a lab. Results arrive through an online portal.
This works reasonably well for initial screening. If you’re curious whether your testosterone is in the normal range or want a snapshot of your thyroid function, a kit can provide that.
The downsides: sample collection errors affect accuracy, reference ranges vary by company, and results come without personalized interpretation. You get numbers—but what do they mean for your body, your symptoms, and your health goals?
Clinical Testing: Accuracy and Context
In-clinic testing involves a venous blood draw analyzed in a certified laboratory. The sample volume is larger, handling is standardized, and quality controls are tighter.
More importantly, clinical testing comes with physician interpretation. Your provider ordered specific tests based on your symptoms. They’ll explain what the numbers mean in context—not just whether values fall inside reference ranges, but whether they’re optimal for you.
The Endocrine Society’s guidelines on testosterone therapy emphasize that diagnosis requires both documented low levels and corresponding symptoms. Numbers alone don’t tell the whole story.
For anyone considering treatment based on results, clinical testing with professional guidance is the appropriate approach.
LIVV Natural’s Approach to Hormone Testing and Evaluation
At LIVV Natural, hormone testing is the starting point—not the endpoint—of care. Here’s what distinguishes our approach:
Comprehensive Panels That Look at the Whole Picture
We don’t test one hormone in isolation. Hormones interact with each other and with other body systems. A man’s low energy might stem from low testosterone—or from thyroid dysfunction, elevated estrogen, or cortisol imbalance. Testing broadly reveals patterns single-marker tests miss.
Our foundational biomarker testing covers sex hormones (testosterone, estrogen, progesterone, DHEA), thyroid function (TSH, Free T3, Free T4, antibodies), adrenal markers (cortisol), and metabolic indicators—giving a complete baseline to work from.
Naturopathic Consultation and Personalized Evaluation
Numbers need interpretation. Our naturopathic doctors specialize in hormone health and take time to understand your full picture—symptoms, history, goals, and lifestyle factors.
We explain what each result means for you specifically. A testosterone level of 450 ng/dL might be “normal” by lab standards but suboptimal for a man with pronounced symptoms. Context matters, and we provide it.
This consultation also identifies root causes. Low testosterone might result from poor sleep, chronic stress, nutrient deficiencies, or medication side effects—not just age. Addressing underlying factors produces better outcomes than hormone replacement alone.
Hormone Treatment Options at LIVV Natural
Once testing confirms a hormone imbalance, treatment planning begins. LIVV Natural offers a range of options matched to individual needs.
Bioidentical Hormone Replacement Therapy
Bioidentical hormones have the same molecular structure as hormones your body produces naturally. They’re available in FDA-approved formulations and can be prescribed in various delivery methods—gels, creams, injections, or pellets.
A Cochrane review of bioidentical hormone therapy for menopausal symptoms found moderate evidence that bioidentical estrogen effectively reduces hot flush frequency in women experiencing vasomotor symptoms.
For women, bioidentical estrogen and progesterone can relieve hot flashes, improve sleep, stabilize mood, and address vaginal dryness. Bioidentical hormone therapy for women at LIVV is individualized based on symptoms and lab values, with regular monitoring to optimize dosing.
Testosterone Replacement Therapy for Men
For men with confirmed low testosterone, testosterone replacement therapy can restore normal levels and relieve symptoms.
Treatment options include weekly or biweekly injections, daily gels or creams, or subcutaneous pellets inserted every few months. Each has advantages depending on preference, lifestyle, and response.
TRT at LIVV includes comprehensive monitoring—not just testosterone levels, but also estradiol (which can rise with treatment), hematocrit (which testosterone can increase), and PSA. We also discuss fertility preservation options for men who may want children in the future.
Natural and Holistic Support
Not everyone needs—or wants—hormone replacement. For mild imbalances or as a complement to HRT, natural approaches can help.
This might include targeted supplements (vitamin D, zinc, magnesium, B vitamins), adaptogenic herbs that support adrenal function and stress response, dietary modifications to stabilize blood sugar and reduce inflammation, or sleep optimization protocols.
Our integrative approach means recommending the least intervention needed to achieve results. If lifestyle changes and supplements can resolve symptoms, we start there.
Peptide Therapy for Hormone Optimization
Peptide therapy uses short amino acid chains that signal specific physiological responses. Certain peptides stimulate natural hormone production rather than replacing hormones directly.
For men, peptides like HCG or gonadorelin can maintain testicular function and natural testosterone production during TRT. Growth hormone-releasing peptides may support metabolism, body composition, and recovery.
Peptides require medical supervision but offer options for those seeking alternatives to traditional hormone replacement.
Men’s Hormone Optimization: What to Expect
Men considering hormone therapy typically arrive with questions about what treatment involves and whether it’s right for them.
Confirming the Diagnosis
Proper diagnosis requires two morning testosterone measurements showing levels below 300 ng/dL (or showing low-normal levels in the context of clear symptoms), along with an evaluation of underlying causes.
We check free testosterone and SHBG because total testosterone can be normal while free testosterone—the biologically active form—is low. We also assess thyroid function, cortisol, vitamin D, and metabolic markers that can affect hormone levels.
Treatment and Monitoring
If testosterone therapy is appropriate, we discuss delivery options and start with standard dosing, adjusting based on response. Most men notice improvements in energy and libido within weeks, with full effects developing over months.
Regular monitoring includes bloodwork to check testosterone levels, estradiol (which we manage if elevated), hematocrit, and PSA. Understanding what optimized testosterone can do helps set realistic expectations—it’s not a miracle cure, but for men with true deficiency, it can meaningfully improve energy, mood, body composition, and sexual function.
Fertility Considerations
Testosterone therapy can suppress sperm production. For men who may want children, we discuss alternatives like HCG or gonadorelin that maintain fertility while improving testosterone levels. Planning prevents problems later.
Women’s Hormone Optimization: What to Expect
Women’s hormone needs vary tremendously based on age, menstrual status, and individual factors.
Perimenopause and Menopause Support
Menopause management at LIVV addresses the full spectrum of symptoms—hot flashes, night sweats, sleep disruption, mood changes, vaginal dryness, and cognitive shifts.
Testing establishes where you are hormonally. Treatment options include bioidentical estrogen and progesterone in forms matched to your needs—oral, transdermal, or vaginal, depending on symptoms and preferences.
Cycle Regulation and PMS
Younger women with irregular cycles, pronounced PMS, or fertility concerns may have underlying hormone imbalances—often involving estrogen/progesterone ratios, thyroid function, or cortisol.
Testing identifies the specific pattern, and treatment might include targeted supplementation, herbal support, or bioidentical progesterone, depending on findings.
Comprehensive Assessment
Women’s hormones don’t exist in isolation. Thyroid dysfunction is more common in women and mimics many menopause symptoms. Adrenal imbalance affects sex hormone production. We assess all systems to find the actual cause of symptoms.
Ongoing Support and Monitoring
Hormone optimization isn’t a one-time fix. Bodies change, hormones shift, and treatment needs adjustment.
Regular Follow-Up Testing
We schedule follow-up labs at appropriate intervals—typically 6-12 weeks after starting or adjusting treatment, then every 6-12 months for stable patients. This confirms treatment is working and catches any issues early.
Treatment Adjustments
If symptoms persist or side effects appear, we modify the approach. Maybe the delivery method isn’t ideal. Maybe dosing needs fine-tuning. Maybe additional factors emerged that need attention.
This iterative process leads to optimization rather than settling for “good enough.”
Long-Term Partnership
Many patients continue with LIVV for years because they value having a provider who knows their history, understands their goals, and stays current with their care. Whether through our Cardiff membership or regular visits to our Little Italy location, ongoing relationships produce better outcomes than episodic care.
FAQs
What are the most common symptoms of a hormone imbalance?
Common hormone imbalance symptoms include persistent fatigue, unexplained weight gain or weight loss, mood swings, anxiety, low mood, poor sleep, reduced libido, and visible changes such as hair thinning, dry skin, acne, or changes in body composition. Because hormones affect metabolism, mood, sexual health, and sleep, symptoms often show up across several systems at once.
How do I know if I should get my hormone levels checked?
Hormone testing makes sense when symptoms persist, start clustering together, or do not improve even after better sleep, diet, exercise, or stress management. Fatigue by itself can have many causes, but fatigue plus weight changes, low mood, poor sleep, or libido changes may point to a hormone-related issue worth testing.
Can a hormone imbalance cause fatigue even if I sleep enough?
Yes. Ongoing fatigue that does not improve with rest is one of the most common warning signs discussed in hormone-related content. Low thyroid function, low testosterone, abnormal cortisol patterns, and other endocrine issues can all affect energy levels even when you are technically getting enough sleep.
Can hormone imbalance symptoms be mistaken for stress or aging?
Yes, and that is one reason hormone issues are often overlooked. Symptoms like low energy, irritability, poor sleep, weight changes, brain fog, and lower sex drive are commonly dismissed as normal aging or stress, even though they can also reflect thyroid, sex hormone, or cortisol imbalances.
What hormones are usually tested when symptoms point to an imbalance?
That depends on the symptom pattern, but common testing may include thyroid markers, testosterone, estrogen, progesterone, cortisol, and related metabolic markers. Men with low-T symptoms are often evaluated with total and free testosterone plus supporting markers, while women with cycle changes or menopause symptoms may need estrogen-, progesterone-, thyroid-, and menopause-related testing.
Is at-home hormone testing accurate?
At-home testing can be useful for early screening, but it has limitations. Sample collection quality, limited marker selection, and lack of individualized interpretation can make results harder to apply in a real treatment setting. Clinical testing is generally more useful when symptoms are significant or when treatment decisions may follow.
Is in-clinic hormone testing better than at-home testing?
For people who want a full evaluation, in-clinic testing is usually the stronger option because it offers standardized sample collection, broader testing panels, and medical interpretation in context. That is especially important when symptoms are ongoing or when you are considering hormone therapy or another targeted intervention.
What are common hormone imbalance symptoms in men?
In men, common symptoms include low energy, reduced libido, erectile changes, lower motivation, mood changes, increased body fat, reduced muscle mass, and sometimes sleep issues or brain fog. These patterns are often associated with testosterone changes, but thyroid and cortisol issues can also contribute.
What are common hormone imbalance symptoms in women?
In women, symptoms often include irregular cycles, mood swings, fatigue, poor sleep, hot flashes, night sweats, vaginal dryness, low libido, acne, hair thinning, and weight changes. Depending on age and timing, these symptoms may relate to perimenopause, menopause, thyroid dysfunction, cortisol imbalance, or other hormonal shifts.
Can thyroid problems look like a hormone imbalance?
Yes. Thyroid dysfunction is one of the biggest reasons people experience fatigue, weight changes, dry skin, hair loss, poor sleep, or mood changes. Because those symptoms overlap with broader hormone imbalance complaints, thyroid testing is often part of a complete hormone workup.
Can a hormone imbalance affect sleep and mood?
Yes. Hormones help regulate stress response, sleep cycles, and neurotransmitter activity, so imbalances can show up as insomnia, restless sleep, irritability, anxiety, low mood, or emotional instability. The overlap between hormone symptoms and mental well-being is one reason testing may help explain symptoms that otherwise feel vague or disconnected.
What happens after hormone testing shows an imbalance?
The next step depends on which hormones are off, how severe the symptoms are, and whether the root issue is thyroid-related, sex-hormone-related, stress-related, or metabolic. A good plan usually moves from test results to a personalized treatment strategy rather than treating one number in isolation. That broader evaluation and follow-up approach is a core part of your blog.
Take the First Step Toward Hormonal Balance
If you’ve been living with symptoms you can’t explain—the fatigue that won’t lift, the weight that won’t move, the mood that won’t stabilize, the sleep that won’t come—hormone testing can provide answers.
LIVV Natural combines comprehensive lab work, naturopathic expertise, and personalized treatment protocols to help you feel like yourself again. Whether you need bioidentical hormones, testosterone optimization, thyroid support, or natural interventions, we build a plan that fits your body and your life.
Stop guessing. Start testing.
Book your hormone evaluation or call 760-454-4600 to schedule a consultation at our San Diego clinics.