Blog
Microplastics and Male Reproductive Health

Plastic particles have now been found in human blood, lungs, placentas, breast milk, and in every single human testis sampled in published research. That last finding is recent and hasn’t received the attention it deserves.
For men concerned about fertility, testosterone, or long-term reproductive function, microplastics are no longer a theoretical environmental concern. They’re a measurable biological reality. The question isn’t whether you’ve been exposed — everyone has. The question is what that exposure is doing inside the body, and what can be done about it.
This post examines the current state of research on microplastics and male reproductive health, including how these particles enter the body, where they accumulate, the mechanisms by which they disrupt testosterone and sperm quality, and practical steps to reduce ongoing exposure. For men already dealing with hormone imbalances or low testosterone symptoms, understanding the environmental piece of that picture matters.
What Are Microplastics — and Why Nanoplastics Are the Bigger Concern
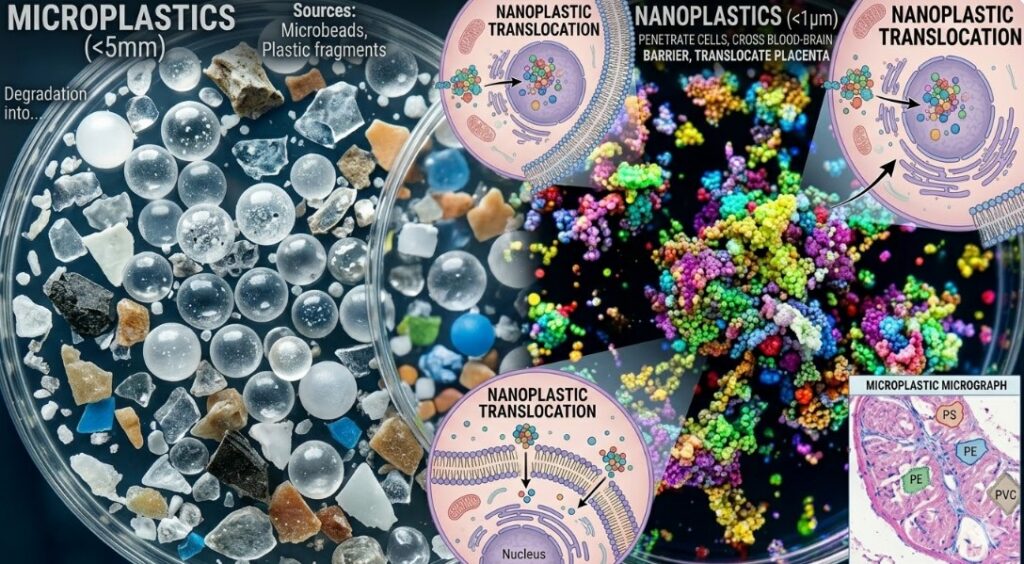
Microplastics are plastic particles smaller than 5 millimeters. They come from two sources: primary microplastics manufactured at that size — like the microbeads once used in exfoliants and toothpastes — and secondary microplastics that form when larger plastic items break down through UV exposure, mechanical wear, and weathering.
The plastic types most commonly found in human reproductive tissue include polystyrene (PS), polyethylene (PE), polyethylene terephthalate (PET), polyvinyl chloride (PVC), and polyamide (nylon). Each has different chemical properties and a different profile of associated endocrine-disrupting chemicals (EDCs) — compounds like BPA, phthalates, PFAS, and flame retardants that leach out of the plastic matrix into surrounding tissue.
Nanoplastics — particles below 1 micrometer — are the fraction that causes more concern in recent research. They’re small enough to cross cellular membranes, penetrate the blood-brain barrier, and translocate across the placenta. Standard filtration systems don’t remove them reliably, and current detection methods can’t yet capture the full extent of human exposure.
What makes this a moving target is that plastic degradation is accelerating. Every piece of plastic ever manufactured is still somewhere in the environment, breaking down into progressively smaller particles. The total body burden of microplastics in humans has been rising year over year, and the research on reproductive consequences is still catching up to the exposure reality.
How Microplastics Enter the Body
Exposure happens through multiple routes simultaneously, which is why complete avoidance isn’t realistic — but meaningful reduction is.
Food and water
Microplastics contaminate seafood through biomagnification — the process by which particles accumulate up the food chain at increasing concentrations. But contamination isn’t limited to seafood. Table salt, honey, fruits, vegetables, and protein sources all test positive. One analysis found microplastics in 90% of protein products tested, including plant-based alternatives. Tap water and bottled water both contain microplastics — with bottled water often showing higher concentrations due to particles shed from the container itself.
Inhalation
Airborne microplastic fibers shed from synthetic textiles, tire wear particles, and degraded outdoor materials are inhaled continuously in urban environments. Indoor air tends to have higher concentrations than outdoor air because synthetic carpets, upholstery, and clothing shed fibers in enclosed spaces. These particles lodge in lung tissue, but smaller fractions enter systemic circulation.
Every day, plastic contact
Plastic food packaging, cutting boards, non-stick cookware, and food containers all shed particles into food — a process that accelerates with heat, scratching, or age of the plastic. Heating food in plastic containers, even those labeled microwave-safe, releases plastic particles directly into food. Non-stick coatings (PTFE/Teflon) are an often-overlooked source — recent research identified PTFE as an underappreciated contributor to male reproductive hormone disruption.
Skin absorption and synthetic clothing
Synthetic fabrics shed microfibers during washing and through direct skin contact. The skin absorbs some fraction of these particles, particularly when clothing is worn for extended periods in warm conditions. Every cycle of a washing machine releases hundreds of thousands of microfibers into wastewater — and into the air of the laundry room.
Where Microplastics Accumulate in Male Reproductive Tissue
A 2023 study from Peking University Third Hospital was the first to confirm microplastics in both human testes and semen simultaneously. MPs were detected in 100% of testis samples, at an average concentration of 11.60 particles per gram of tissue. Polystyrene was the dominant polymer in testicular tissue, while polyethylene and PVC predominated in semen. Particle sizes ranged from 20 to 100 micrometers — small enough to cross biological barriers that were previously thought to be protective.
Semen is also consistently affected. A 2025 study found microplastics in 34 of 45 semen samples analyzed, with PET as the most common polymer at 35.9% of particles detected. Men with PET in their semen showed lower sperm progressive motility — approximately 21% versus 35% in unexposed men. Fifteen distinct polymer types were identified across samples.
Beyond reproductive tissue, a systematic review published in 2025 on medRxiv confirmed MPs in human blood, placenta, lungs, uterus, testes, semen, breast milk, and ovarian follicular fluid. The review linked in vivo microplastic exposure to cardiovascular events, reproductive damage, inflammatory responses, and oxidative stress — making clear that the effects extend well beyond the reproductive system.
How Microplastics Disrupt Testosterone and Male Reproductive Health
Finding plastic in testicular tissue is one thing. Understanding what it does there is the more important question — and the research is now starting to answer it.
Testosterone suppression via the steroidogenesis pathway.
Chronic exposure to polystyrene microplastics at environmental concentrations caused reduced serum testosterone, LH, and FSH — alongside altered testicular morphology, decreased sperm viability, and increased sperm abnormality. The mechanism involved downregulation of the LHR/cAMP/PKA/StAR steroidogenesis pathway — the chain of molecular events Leydig cells use to produce testosterone in response to LH signaling from the pituitary.
Oxidative stress in Leydig cells.
Polystyrene microplastics suppress glutathione peroxidase 1 (GPX1), a key antioxidant enzyme in testicular tissue. This creates localized oxidative stress in Leydig cells — the cells responsible for testosterone production — leading to a reduction in testosterone, independent of the hormonal signaling pathway. In other words, even if LH signaling is intact, oxidative damage to Leydig cells can suppress testosterone output directly.
Testosterone binding and receptor blockade.
Polyamide microplastics — the kind shed from nylon sportswear, packaging, and textiles — bind directly to testosterone molecules, reducing their intracellular availability. They also block androgen receptor nuclear translocation, preventing testosterone from signaling at the cellular level even when serum levels appear normal. This has direct implications for how testosterone deficiency is diagnosed and interpreted in men with significant plastic exposure.
Mitochondrial dysfunction and apoptosis.
Chronic PS-MP exposure induced testicular oxidative stress, mitochondrial dysfunction, and apoptosis of Leydig cells via the BAX/BCL2 pathway — programmed cell death that permanently reduces testosterone-producing capacity. Mitochondrial damage is a particularly concerning mechanism because it compounds over time rather than resolving when exposure stops.
EDCs carried by plastic compounds add another layer of complexity. Microplastics carry and leach endocrine-disrupting chemicals, including phthalates, BPA, PFAS, and flame retardants, into surrounding tissue. These chemicals disrupt testosterone synthesis, thyroid signaling, cortisol regulation, and the broader reproductive hormone cascade. BPA in particular is well-established as an anti-androgenic compound — it competes with testosterone at androgen receptors and suppresses its production through multiple pathways.
Microplastics and the Global Sperm Count Decline
Global average sperm counts have fallen by more than 50% over the past 40 years. That’s one of the most consistent and replicated findings in reproductive medicine — confirmed across dozens of studies in North America, Europe, and Australia. The decline is ongoing, and its causes are still being worked out.
Microplastics are now one of the leading candidates for explaining part of that trend. The timeline matches: industrial plastic production scaled up in the 1950s and 1960s, and the sperm count decline became measurable roughly a generation later — consistent with the time it would take for widespread environmental contamination to translate into measurable reproductive effects.
Microplastics reduce adult sperm production and alter prenatal male genital development in animal studies, and link climate change, environmental toxins, and EDCs, including BPA and phthalates, to declining global sperm quality. The authors described the intersection of these factors as an accelerating concern for male reproductive medicine.
The developmental window matters too. Exposure beginning in early development through adulthood impaired male reproductive function in mice across multiple life stages. MPs were detected in the sperm of males as young as 10 years old in a referenced 2024 human study — suggesting that exposure during development may set reproductive trajectories well before a man is aware of any fertility concern.
This doesn’t mean microplastics are the sole cause of sperm count decline. Obesity, sedentary behavior, poor diet, heat exposure, and other environmental toxins all contribute. But the evidence that microplastics play a direct mechanistic part — through multiple pathways, at concentrations found in everyday life — is now strong enough that it can’t be treated as speculative.
Microplastics, Penile Tissue, and Erectile Dysfunction
The connection between microplastics and erectile dysfunction is newer and deserves its own section because the finding is striking.
A study published in IJIR examined penile tissue from men undergoing surgery for erectile dysfunction and found microplastics in 80% of samples. The most common polymer types were polyethylene terephthalate (PET) — the plastic used in water bottles, food containers, and polyester clothing — and polypropylene (PP), used in packaging and household items. These are among the most common plastics in daily use.
The proposed mechanisms connect to what’s already known about microplastic toxicity: local inflammation in vascular tissue, endothelial dysfunction from oxidative stress, and EDC-mediated hormonal disruption that reduces libido and the hormonal drivers of erectile function. Whether microplastic accumulation in penile tissue is a cause or a marker of broader vascular and hormonal compromise isn’t fully established — but the presence of plastic in that specific tissue, in men presenting with ED, is a finding worth taking seriously.
For men managing erectile dysfunction through hormone optimization or peptide therapy, addressing the oxidative and inflammatory environment created by ongoing microplastic exposure may be as relevant as the hormonal intervention itself.
How to Reduce Microplastic Exposure: What Actually Makes a Difference
Complete avoidance isn’t possible. Microplastics are in the food supply, the water supply, and the air. But the cumulative exposure load matters — and meaningful reductions are achievable with targeted habit changes.
Filter your drinking water
Both tap and bottled water contain microplastics, but high-quality filtration removes a large fraction of them. A reverse osmosis filter or a pitcher filter with a 1-micron or smaller pore size will reduce MP concentrations more than standard carbon filters. If you use bottled water regularly, switching to filtered tap water in a glass or stainless steel container immediately reduces one of the higher-exposure routes.
Overhaul how you store and heat food
Never heat food in plastic containers — even those labeled BPA-free or microwave-safe. The heat accelerates particle and chemical release into food. Switch to glass, ceramic, or stainless steel for food storage and reheating. Discard scratched or worn plastic containers, as degraded plastic sheds particles at higher rates than intact surfaces.
Replace plastic cutting boards
Plastic cutting boards shed an estimated 50 million microplastic particles per year into food during normal use. Wooden or bamboo boards are the direct replacement. This is one of the higher-exposure kitchen sources that most people don’t think about.
Avoid non-stick cookware
PTFE-coated (Teflon) pans shed particles into food, particularly when the coating is scratched or the pan is overheated. Cast iron, stainless steel, and ceramic-coated cookware are the practical alternatives. Non-stick coatings also carry PFAS compounds — the same class of chemicals linked to testosterone reduction and thyroid disruption in occupational and environmental studies.
Choose natural fibers when possible
Synthetic clothing — polyester, nylon, spandex — sheds microfibers continuously during wear and washing. Choosing cotton, wool, linen, or hemp for everyday clothing reduces dermal and inhalation exposure. For washing, a microfiber-catching laundry bag or washing machine filter traps fibers before they enter wastewater and recirculate as airborne particles when the machine is running.
Reduce seafood from high-contamination sources
Shellfish — mussels, oysters, clams — tend to have higher microplastic concentrations than finfish because they filter-feed directly from water. This doesn’t mean eliminating seafood, which has genuine nutritional benefits for hormone production and sperm health. But sourcing matters, and diversifying protein sources reduces reliance on the highest-exposure options.
FAQ
Can microplastics affect male fertility?
Yes, that is what the current research increasingly suggests. Microplastics are associated with reduced sperm quality, impaired motility, higher oxidative stress, and damage to the male reproductive environment. They do not appear to affect fertility through only one pathway, but through several at once, including inflammation, oxidative damage, and endocrine disruption.
Do microplastics lower testosterone?
They may. Research has linked chronic exposure to certain microplastics, especially polystyrene microplastics, with lower testosterone levels and impaired steroid hormone production. The proposed mechanisms include oxidative stress in Leydig cells, disruption of testosterone synthesis pathways, and interference from endocrine-disrupting chemicals carried by plastics.
Have microplastics been found in human semen and testicular tissue?
Yes. Recent human studies have reported microplastics in testicular tissue and semen samples, which is one reason this topic has become far more serious in male fertility discussions. These findings do not prove that every fertility issue is caused by microplastics, but they do confirm that reproductive tissues are not protected from exposure the way researchers once assumed.
How do microplastics harm sperm health?
Microplastics appear to harm sperm health by increasing oxidative stress, promoting inflammation, and disrupting the hormonal systems involved in sperm production and maturation. Over time, that may contribute to lower motility, more abnormal sperm forms, and weaker overall reproductive function. Researchers are also looking at how plastic-associated chemicals may worsen those effects by adding another layer of endocrine disruption.
How can men reduce microplastic exposure in everyday life?
The most practical steps are to stop heating food in plastic, switch to glass or stainless steel for food and water storage, reduce bottled water use, replace damaged non-stick cookware, use fewer plastic cutting boards, and choose natural fibers more often when possible. Complete avoidance is not realistic, but lowering daily exposure across food, water, air, and household contact can meaningfully reduce total burden over time. Human exposure happens through food, water, and inhalation, so small habit changes across all three routes matter more than focusing on only one source.
How LIVV Natural Approaches Microplastic-Related Male Health Concerns
No clinic can remove microplastics from your body — that technology doesn’t exist yet. What a naturopathic practice can do is assess the downstream effects of ongoing exposure and address them directly: the oxidative stress, the hormonal disruption, the mitochondrial damage, and the inflammatory burden that plastic accumulation creates.
The starting point at LIVV is testing. Foundational biomarker panels cover testosterone (total and free), LH, FSH, SHBG, thyroid hormones, DHEA, and inflammatory markers — the full hormonal picture that microplastic research has identified as most affected. Testing gives a baseline and makes it possible to measure whether interventions are working.
On the treatment side, several of LIVV’s IV therapies directly address the biological pathways that microplastics disrupt. Glutathione IV therapy counteracts Leydig cell oxidative stress — the same mechanism by which PS-MPs suppress testosterone via GPX1 suppression. Glutathione is the primary antioxidant defense in testicular tissue, and IV delivery restores it faster than oral supplementation.
NAD+ IV therapy addresses the mitochondrial dysfunction that chronic microplastic exposure produces. Leydig cell apoptosis driven by mitochondrial damage is one of the mechanisms identified in animal research as a sustained testosterone suppressor, and NAD+ is the primary substrate for mitochondrial repair and energy metabolism. For men dealing with fatigue, low drive, and declining testosterone that doesn’t fully respond to standard interventions, mitochondrial support is often the missing piece.
Ozone therapy provides systemic anti-inflammatory support that counters the inflammatory response microplastics trigger in testicular and vascular tissue. High-dose vitamin C and antioxidant IV drips round out the oxidative stress management side of the protocol.
For men whose hormone testing shows low testosterone or disrupted hormonal ratios, hormone optimization at LIVV addresses the functional deficit directly — whether through testosterone replacement, peptide-based growth hormone optimization, or natural hormone support protocols. The goal is to address both the environmental burden and the hormonal outcome it produces.
LIVV Natural operates out of two San Diego locations: LIVV Little Italy and LIVV Cardiff, a members-only longevity club. A naturopathic consultation in San Diego is the right starting point if you want to get a full picture of where you stand and build a protocol that’s specific to your labs and your goals — not a generic approach.
If your testosterone has been declining, your energy is lower than it should be, or you’re dealing with fertility concerns, the environmental piece deserves the same attention as the clinical interventions. The research on microplastics and male reproductive health is no longer preliminary — it’s consistent, mechanistically explained, and growing.